What is Psoriatic Arthritis?
Psoriatic Arthritis (PSA) is a specific type of arthritis that is linked with Psoriasis. Psoriasis is a chronic skin condition that causes scaly, red rashes and thick pitted fingernails. While PSA is similar to other types of arthritis (inflammation and joint swelling), it does tend to affect fewer joints than some other arthritis’ like Rheumatoid Arthritis.
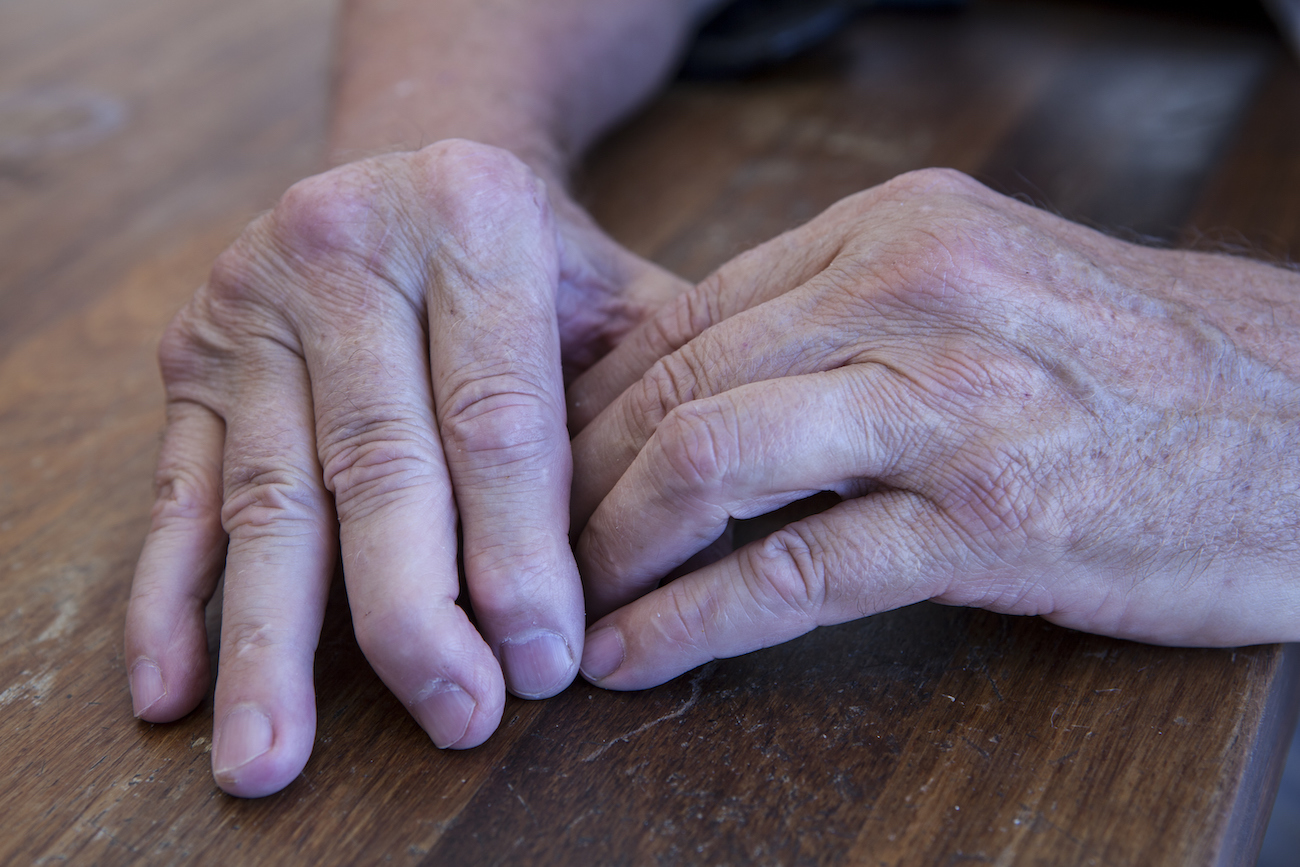
Symptoms include:
- Inflamed, swollen, and painful joints, often in the fingers and toes
- Foot pain where tendons and ligaments attach to the bones, especially at the back of the heel
- Lower back pain
- Nail changes – nails can become pitted (or dented), crumble or separate from the nail beds
- Eye inflammation associated with uveitis which causes redness and blurry vision
- Joints can become deformed from chronic inflammation
How is Psoriatic Arthritis Diagnosed?
PSA is easiest to confirm if psoriasis is already present. Diagnosis is more difficult without skin symptoms.
- Physical exam to look at joint swelling, fingernail pitting or flaking.
- Erythrocyte Sedimentation Rate – this test determines the rate at which red blood cells settle to the bottom of a tube within an hour. A faster rate may indicate a disease, such as Lupus, but the sedimentation rate isn’t specific for any one disease.
- Imaging – X-rays, CT scans, ultrasound, MRI and skin biopsies may all be used to diagnose
Treatment for Psoriatic Arthritis
Your provider will consider many factors when determining the best treatment for you. Symptoms, age, overall health, health history and the severity of your condition will all play a part in choosing the best treatment.
With psoriatic arthritis, the skin condition and joint inflammation may require treatment based on your unique case.
- NSAIDs (nonsteroidal anti-inflammatory medicines) to ease symptoms.
- Corticosteroids for inflammation.
- Immunosuppressive medications such as methotrexate may be used if NSAIDs do not work.
- Biologic medicines can significantly assist pain management, reducing inflammation and overall quality of life. Your provider may recommend one of these treatments; infusion drugs can be administered in our in-office infusion suites.
- Physical and occupational therapies can assist in easing pain and making everyday tasks easier.
Lifestyle modifications may help manage your disease, such as maintaining a healthy weight, exercising regularly, smoking cessation, limiting alcohol use and avoiding overtaxing yourself in everyday activities.